By akshita · February 11, 2026
You are aware of the burden of your legacy systems every day. The slowness of workflows, fragmentation of data, and inflexible technology make it difficult to provide support to patients, payers, and partners. Moreover, you have to improve outcomes, protect data, and support new digital experiences simultaneously. The difference between what your systems provide and what your organization necessitates is continually increasing.
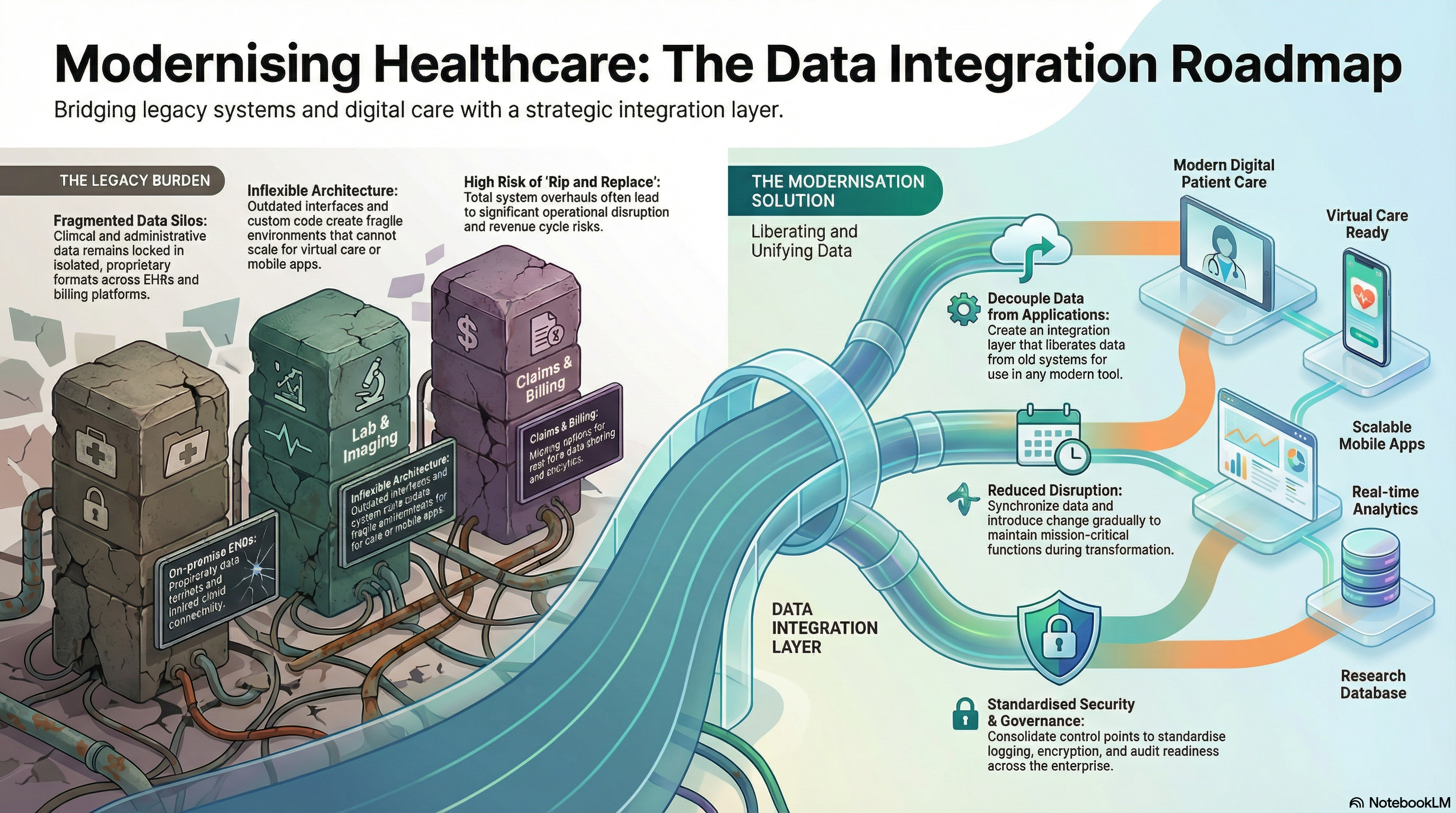
Upgrading your old guardians of health care through the use of data integration allows you to dispel that gap with less risk and more control. Rather than taking out every system, you link them, synchronize data, and gradually introduce change. You keep the good stuff while getting ready for what’s next.
Such a path is of great help to your employees in their day, to, day work. It acknowledges the intricacy of your setup from EHRs and lab systems to claims platforms and analytics tools. If you have a good integration plan, you will be able to modernize at a higher speed, lower the level of disruption, and share the data usage benefits within your whole organization.
What Are Legacy Healthcare Systems
Legacy healthcare systems are the clinical and administrative applications that have been central to your operations for many years. You rely on them for essential functions, yet they were not designed to meet the digital health requirements of today. Frequently, they operate on old architectures, employ outdated interfaces, and lock data into isolated formats.
You can spot legacy systems in several areas:
- On-premise EHRs and practice management platforms.
- Laboratory and imaging systems with proprietary data formats.
- Claims, billing, and revenue cycle applications have very few integration options.
- Care management or population health tools are limited to specific platforms.
These systems enable your core processes to function, but they are not very adaptable to change. If you attempt to link them to new tools, mobile apps, or analytics environments, you will encounter fragile interfaces, custom code, and manual workarounds.
Modernizing legacy healthcare systems acknowledges that you cannot overhaul everything at once. Rather, you concentrate on modernizing legacy healthcare systems through data integration so you can continue to perform mission-critical functions while constructing a more versatile environment around them.
Why Modernization Is Critical for Healthcare Organizations
Your company is at the core of a complicated network of patients, providers, payers, and partners. All of them rely on accurate, up, to, date data. Outdated platforms and point-to-point interfaces are a major barrier to scaling digital care models, value-based programs, and getting real-time insights.
There are several reasons why modernization is essential.
Support new clinical and business models.
Virtual care, remote monitoring, and team-based care necessitate the uninterrupted availability of integrated patient data from different care settings. If all these new capabilities require separate interfaces to an old system, your costs will increase, a nd your deadlines tend to slip. The way healthcare data is integrated nowadays enables your teams to make the right data available only once, in a reusable manner, so they can support new workflows without having to reconstruct the whole IT stack every time.
Improve care coordination and patient experience
Patients nowadays wish for a connected experience. They expect their doctors to have access to their medical history, medication, and test results without being asked repeatedly or waiting too long. When the data is stored in isolated systems, the staff has to manually perform reconciliations, print out reports, and duplicate data entries. Healthcare data integration as part of digital transformation allows you to create one comprehensive, reliable patient record that makes it possible to make quicker decisions and fewer care transitions.
Strengthen compliance and security posture
The regulatory landscape keeps evolving, and with it, the compliance requirements. You must have a clear picture of who is accessing what data, the movement of the data, and the protection measures in place. In fact, outdated user interfaces and homemade scripts are a major threat to your security because they are very difficult to supervise and trace. Healthcare data integration for legacy systems helps you consolidate control points, standardize logging, and diminish undocumented data flows.
Enable scalable analytics and innovation
Investments are being made into analytics platforms, population health tools, and quality reporting. However, if the data is not integrated, these investments will not deliver the expected results. Transforming legacy healthcare IT systems by modern integration will provide your analytics teams with cleaner and more up, to, date data. Besides, it will prepare you for the eventuality of use cases such as real-time alerts, predictive models, and advanced quality programs.
Role of Data Integration in Modernizing Legacy Systems
Data integration is a critical part of modernizing old healthcare systems. It is not merely about transferring the data from one system to another. It is about setting the standard of how your organization will share, govern, and utilize information throughout the whole ecosystem.
Decouple data from legacy applications
It is not your intention to hold onto every old system for eternity. What you want is to liberate your data from those systems in such a way that you can use it anywhere. Continuing the modernization of old healthcare systems through data integration enables you to differentiate data from applications. You establish an integration layer that simultaneously supports existing systems and new systems that you introduce gradually.
Translate across standards and formats
In your environment, you have HL7, FHIR, X12, flat files, proprietary APIs, and custom exports. The integration project can be a translation exercise each time. With modern healthcare data integration, you can handle these differences consistently. You map, transform, and normalize data so downstream systems get the data in the format they expect.
Orchestrate data flows across the enterprise
You are looking for something beyond just point-to-point connectivity. You want orchestrated workflows that support event-driven processes. For instance, you could send an admission event from a legacy EHR to care coordination tools, population health platforms, and notification services. Data integration provides the routing, rules, and monitoring to manage those flows with control and transparency.
Provide a foundation for future upgrades
When you see the integration as a core capability rather than a string of one-off projects, you are preparing yourself for the future. Changing healthcare IT systems will be less of a headache as your integration layer will be taking care of a lot of the complexity. New applications will be able to use the existing integration fabric instead of requiring custom work every time.
Key Benefits of Modernizing Legacy Systems With Data Integration
Upgrading old healthcare systems through data integration helps in enhancing operations, clinical performance, and strategy. However, these advantages are not solely due to technology. These outcomes derive from a combination of the best platforms and a well-defined modernization strategy.
Reduced disruption during transformation
Completely replacing a system usually brings about patient care and revenue cycle risks. Concentrating on integrating data in health care legacy systems, you don’t have to make a dramatic change. Firstly, you can continue your existing workflows, then slowly transfer the data and features to newer platforms, and finally, at each stage before moving forward, you can verify the changes.
Better use of current investments
You have at least two platforms, each of which is capable of performing certain functions. Therefore, before throwing them away, you could consider extending their value with a modern healthcare data integration. You don’t have to replace them right away by integrating the data for a healthcare system modernization, which enables you to consolidate the information from within those systems into a more helpful whole.
Faster delivery of new capabilities
Any time you have a reusable integration layer, each new project goes faster. You are not required to figure out how to connect to your core platforms again every time. That speeds up patient engagement tools, payer integrations, quality reporting, or partner connections type of projects.
Improved data quality and consistency
Rarely, the data from legacy systems is dirty and contains duplicate records, inconsistent codes, and incomplete fields. Enterprise integration enables you to carry out validation, standardization, and enrichment at the integration layer. Thus, the data that the systems get are more accurate and ready for use, which can lead to better analytics and safer clinical decisions.
Stronger security and governance
By consolidating the interfaces onto a modern integration platform, you are effectively shrinking your attack surface. You get a structured access control, encryption, auditing, and monitoring functionalities all in one place. This helps you with internal governance, external audits, and regular risk management activities.
Challenges and Considerations During Modernization
Modernizing legacy healthcare systems by data integration is a smart move. It gets involved with technology, process, and culture. To be successful, you need to foresee the problems and make a plan for them beforehand.
Complexity of legacy systems
Legacy platforms may have custom code, undocumented workflows, and tightly coupled interfaces. Simple interface diagrams rarely reveal the real situation. You need to take a formal evaluation of your current integrations, data flows, and dependencies. This evaluation directs your healthcare system modernization strategy and safeguards you from unexpected downtime.
Resource and skill constraints
Your in-house teams are responsible for running operations and providing support daily. They probably do not have the time or the specialized skills necessary to create and use modern healthcare data integration platforms. You have to decide which areas to develop internal capabilities and which to hire integration consultants who are conversant with healthcare standards and workflows.
Managing change across stakeholders
Integration changes will have an impact on the different groups of people around the hospital such as the clinicians, IT staff, revenue cycle teams, and external partners. They each need to know exactly what, where, and how these changes are going to be made and at what time and how these changes are going to make their lives easier. If a communication channel and change management aren’t set up properly, then the change resistance, workarounds, or mistrust are almost inevitable.
Data governance and ownership
Questions around ownership rights, access rights, and usage will become more and more visible as you integrate even more data. You need to have governance mechanisms that are able to answer the question of who is the caretaker of each data domain, who has the privilege to get which data, and how the data is being used in combination with clinical, operational, and analytics cases.
Balancing speed with risk
There is a demand to demonstrate the outcomes of your efforts rapidly, even though you have to be careful not to disrupt the financial performance and patient care. Any healthcare IT system upgrade through integration needs to be mapped out in such a way that it not only catches some quick wins, but it also ensures that the whole system will remain stable for a long time. Separate release, proper testing, and having a clear rollback plan are must-haves.
Best Practices for Successful Legacy System Modernization
A methodical and well-organized plan can help you to map the integration efforts with business value. The afore, mentioned practices will not only fortify your modernization strategy but also lessen the element of risk.
Start with a clear vision and outcomes
Before you choose the tools or design the interfaces, make sure that you know what success looks like. Help the process of modernizing the legacy healthcare systems by data integration to specific outcomes. For instance, improved care coordination, quicker onboarding of partners, or enhanced analytics capabilities. Turn these outcomes into a priority guide and use them to measure progress.
Assess and map your current environment
It is a good practice to write down your current systems, interfaces, data flows, and issues. You should take into account different domains such as clinical, financial, and operational. Which areas of your business are the ones that generate the most friction, have the most manual work, or where are the redundant integrations? With this evaluation, you will be able to build a roadmap for the legacy healthcare system modernization.
Adopt a centralized integration strategy
Abandon point, to, point connections that are slow and hard to manage and integrate. Deploy a centralized integration platform or hub that can handle various standards like HL7, FHIR, and X12. Your healthcare data integration strategy for legacy systems should be aligned with a centralized, unified platform facilitating transformation, routing, and monitoring.
Prioritize data standardization and quality
Integration without standardization makes the problem even more complicated. Agree on common data models, code sets, and reference data that apply to all systems. Let your integration layer be the enforcer of those standards. The aim of a modern healthcare data integration is to raise data quality, not merely to increase the speed of data movement.
Design for security and compliance from day one
Security and privacy requirements have to be the main focus of your integration strategy. Make sure that the implementation of access control, encryption, auditing, and alerting is done at the core capabilities level rather than as add-ons. Combine internal security policies and external regulations in your approach to risk reduction and audit readiness support.
Use phased modernization and parallel runs
Large cutovers are quite risky. Hence, plan a phased migration of the old integration and new one being run in parallel for a certain period. It allows you to compare outputs, identify problems at an early stage, and gain the trust of end users. Integrated healthcare system data for modernization enables these parallel paths by delivering consistent data between old and new processes.
Align IT, clinical, and business stakeholders
Modernization choices should mirror the requirements of people who use and rely on the systems daily. Include clinical leaders, operations leaders, and revenue stakeholders in governance structures. Involve their ideas to set priorities, define success metrics, and evaluate trade, offs during healthcare IT systems upgrading.
Partner with healthcare integration experts
Healthcare integration is not a regular IT problem. It needs an understanding of standards, workflows, and compliance requirements. A partner experienced in modern healthcare data integration will be a great help in your fast and risk-free progress. They bring to the table reusable patterns, validated architectures, and proven delivery models.
Conclusion
You are under increasing pressure from patients, payers, regulators, and partners. Your legacy systems are what keep your organization running, but they also put a cap on your options. Modernizing legacy healthcare systems with data integration is a smart way to get your organization moving again while not completely disrupting your existing operations. You maintain stability while gradually moving towards a more connected, flexible, and data-driven environment.
With the proper strategy, you no longer have to put out fires every time a new integration is required. Instead, you can build an integration foundation that supports your organization’s continuous improvement. So you capitalize on the data that was once scattered as anetwork asset. You make things easier and more comprehensible for your folks. You also find time for new inventions without compromising the dependability of your operations.
Vorro is in the business of helping healthcare organizations modernize through smart integration. Our integration platform and services primarily deal with healthcare data integration of legacy systems, healthcare IT system upgrade with minimal disruption, and healthcare system modernization through integrated data that reflects true clinical and business outcomes.
Should you decide to advance with legacy healthcare system modernization, we invite you to schedule a strategic discussion with Vorro and synchronize your integration plan with your main goal.
FAQs
How do you initiate the modernization of legacy healthcare systems through data integration?
You first conduct a thorough analysis of your existing systems, interfaces, and data flows. After that, you determine your desired outcomes, decide on the integration use cases, and pick an integration platform that meets your standards and security needs. Initial successes are usually achieved by addressing highly problematic workflows that affect both clinicians and operations.
What is the function of FHIR in the modernization of legacy healthcare systems?
FHIR sets a fresh standard for the representation and exchange of healthcare data. In the course of modernizing legacy healthcare systems, you may leverage your integration platform to convert between traditional standards like HL7 and the more recent FHIR, based APIs. Thus, you are able to back up the latest applications without making the immediate overhauling of all legacy systems mandatory.
How does data integration reduce the risk of upgrading healthcare IT systems?
A reliable integration layer makes it possible for you to keep using old and new systems at the same time, to slowly divert traffic, and to check the results before the full cutover. Besides, it helps centralize monitoring as well as error handling. Such a framework drastically lowers the chances of outages, data loss, or disruption of workflows when major system upgrades are carried out.
What internal teams should be involved in healthcare data integration for legacy systems?
In addition to IT, clinical leadership, and operations, you should also include the revenue cycle, compliance, and security teams. Each team can shed light on requirements, limitations, and criteria for success. This cross-functional engagement ensures that your integration strategy will be not only technically viable but also aligned with real-world workflows.
How do you gauge the success of integrated data when it comes to healthcare system modernization?
Success is basically determined by the achievement of outcomes that are most valuable to your organization. For instance, these could be less manual work for the employees, quicker onboarding of partners, more accurate and timely reporting, improved data quality for analytics, and fewer integration incidents. You should establish these criteria before and keep monitoring them during your modernization journey.
Vorro is your partner when it comes to modern healthcare data integration and legacy healthcare system modernization. We help healthcare organizations that are looking for a practical way of making progress without taking excessive risks. Check out how Vorro can assist you in aligning your integration, results, and mission at Vorro.
