By manoj.kumar · February 7, 2026
You sit on more data than ever from clinical, financial, operational, and patient engagement systems. You also feel daily pressure to connect it. Quality programs, risk contracts, care coordination, and digital front door efforts all depend on consistent data flows. Yet every project runs into the same barriers. The core problem is clear. You face persistent data integration challenges in healthcare that slow progress and raise risk for large enterprises.
When your teams try to connect EMRs, claims systems, CRM, scheduling, and analytics platforms, the effort often drags on. Interfaces become brittle. Reports lose trust. Security teams push back. Vendors blame each other. Leaders lose momentum. You need a more structured view of health system data integration issues and a clear strategy to move through them with confidence.
Overview of Data Integration in Healthcare
Data integration in large healthcare systems focuses on creating a consistent, governed flow of information across clinical, financial, and operational systems. You need the right data, in the right place, at the right time, with clear ownership and controls. The real goal is not the interface itself. The goal is reliable outcomes for patients, clinicians, and business leaders.
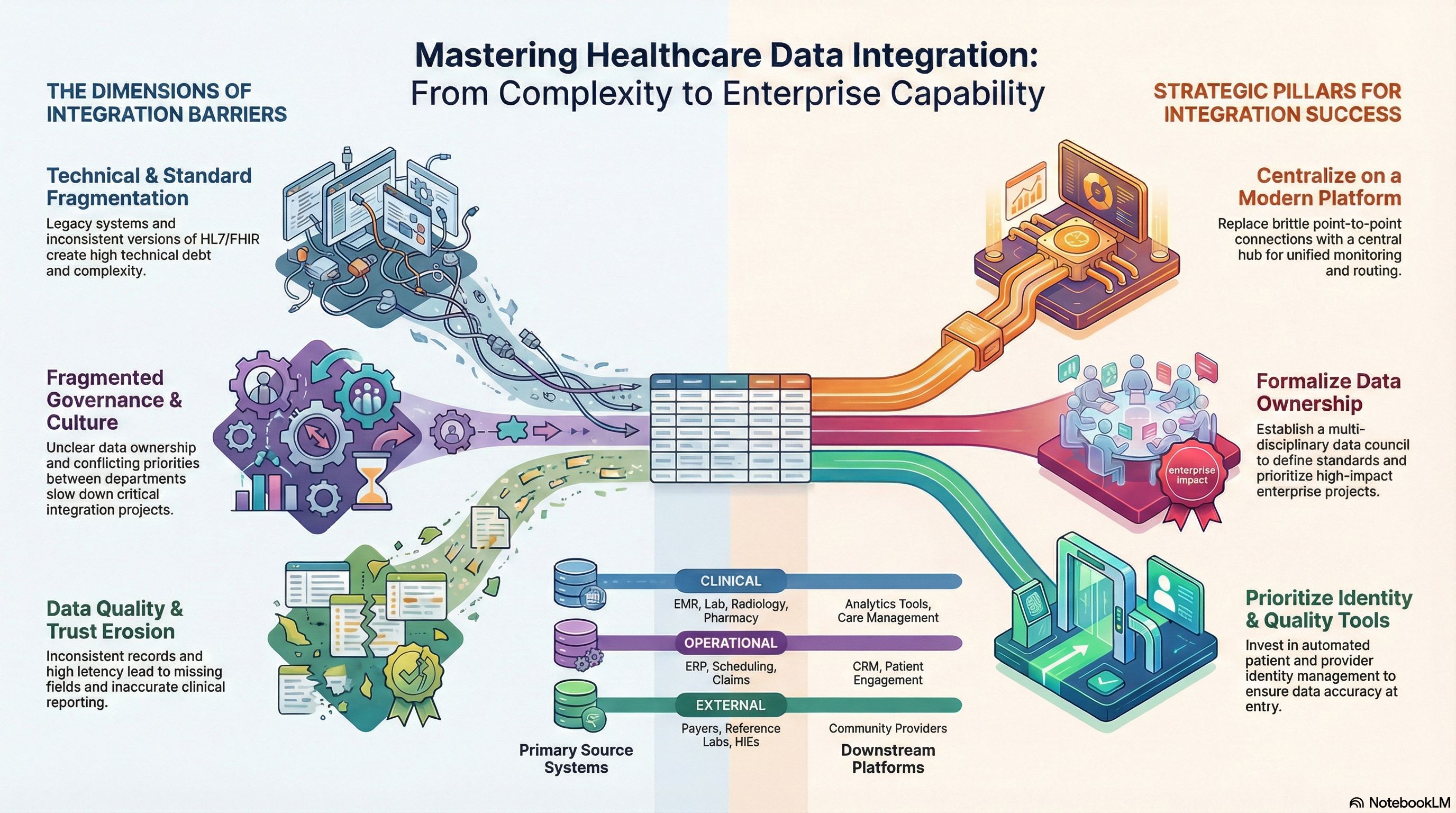
At its core, data integration connects:
• Source systems such as EMRs, lab, radiology, pharmacy, claims, and ERP
• Downstream platforms such as analytics tools, care management, CRM, and patient engagement
• External partners such as payers, HIEs, reference labs, and community providers
When these flows work, care teams see complete patient context. Revenue and clinical operations align. Leadership trusts metrics. When they do not, you face significant healthcare data integration obstacles that ripple across quality, cost, and experience.
Data integration challenges in healthcare show up across four major dimensions. Technology, organization, data quality, and security. Each one needs specific attention and an intentional strategy.
Common Challenges in Large Health Systems
Large healthcare system data integration efforts rarely fail for a single reason. They stall under the combined weight of scale, complexity, and fragmentation. The same patterns repeat across regions, service lines, and programs.
Common health system data integration issues include:
• Multiple EMRs and ancillary systems after mergers and acquisitions
• Different standards and versions across facilities and partners
• Shadow IT solutions that bypass enterprise oversight
• Inconsistent governance around data ownership and definitions
• Manual workarounds that hide broken integrations
• Limited observability into interface health and data flows
• Conflicting priorities between IT, operations, and clinical leaders
Each new integration project tries to work around these issues. Over time, you inherit a web of point-to-point connections and partial solutions. This adds more healthcare data interoperability challenges and increases operational risk.
To move forward, you need a clear breakdown of the underlying technical, organizational, and data quality barriers. That clarity lets you sequence work and invest in the right platforms and processes.
Technical Challenges: Systems, Standards, and Interoperability
Technical complexity sits at the center of most data integration challenges in healthcare. The number of systems, formats, and standards in a large enterprise creates friction on every project.
Fragmented Systems Across the Enterprise
Large health systems often run multiple EMRs, billing platforms, lab systems, radiology platforms, and specialty solutions. Each system has its own data model, interface engine, and configuration history. You inherit these differences from prior acquisitions and local decisions.
As a result, large healthcare system data integration efforts must:
• Connect systems that were never designed to work together
• Support multiple workflows for the same clinical process
• Maintain different instance configurations over time
Without a central integration strategy, your team spends time chasing exceptions and reworking connections instead of delivering new value.
Inconsistent Standards and Interfaces
Healthcare data interoperability challenges often stem from partial or inconsistent use of standards. Different vendors and facilities use different versions of HL7, FHIR, and proprietary APIs. Even within one standard, field use and code sets vary between sites.
This creates healthcare data integration obstacles such as:
• Different mappings for the same clinical concept across systems
• Inconsistent identifiers for patients, providers, and locations
• Variable support for FHIR resources and operations
• Limited documentation for vendor specific extensions
You then need custom transformation logic, error handling, and reconciliation rules for each connection. The technical debt grows with every project.
Legacy Integration Patterns and Tools
Many integration layers in large systems rely on older interface engines, file drops, and manual ETL jobs. These patterns struggle to support real time needs from digital and analytics teams.
Legacy approaches lead to:
• Limited observability into message flow and failures
• Long lead times to build or change interfaces
• Duplicate transformation logic across projects
• Difficulty managing version control and regression testing
As your digital strategy grows, these technical limits slow adoption and raise the operational cost of every new integration.
Organizational Challenges: Governance, Compliance, and Culture
Technology is only one part of the story. Many of the toughest data integration challenges in healthcare are organizational. Governance, accountability, and culture shape how fast and how safely you integrate data.
Weak or Fragmented Governance
Healthcare data governance challenges appear when ownership of data domains is unclear. Clinical, financial, and operational leaders often define data differently. Each group optimizes for its own reporting or workflow needs.
Without strong governance you see:
• Conflicting definitions for key measures
• Disputes about source of truth for datasets
• Slow decision making on integration priorities
• Uncoordinated extract and interface requests to IT
The result is more health system data integration issues such as inconsistent analytics and duplicated data flows. Every team builds its own version of the truth.
Compliance and Risk Concerns
Privacy and security rules shape every data decision in healthcare. Large systems need strong control over PHI, access, consent, and retention. Security leaders carry real accountability for risk.
When integration work does not align with clear policies and controls, security and compliance teams slow or stop projects. From their view, fragmented data flows increase exposure. You then face healthcare data integration obstacles such as:
• Long review cycles for new interfaces and data feeds
• Reluctance to share data across affiliates or partners
• Limited support for cloud analytics or external platforms
This friction often reflects underlying gaps in governance and architecture, not resistance to integration itself.
Cultural Misalignment and Competing Priorities
Integration projects cross many teams. IT, clinical operations, finance, quality, and population health. Each group has its own workflows, constraints, and success metrics.
When priorities differ, you see:
• Limited clinical engagement in technical design decisions
• Business units funding point solutions without enterprise alignment
• Resistance to standardization of workflows or data definitions
• Low adoption of integrated tools after go live
These organizational factors turn technical challenges into persistent healthcare data interoperability challenges that slow strategic programs across the system.
Data Quality and Security Challenges
Even with solid interfaces and governance, you still need accurate, timely, and secure data. Data integration challenges in healthcare often show up here first. Users notice missing fields, wrong values, or outdated information before they notice elegant technical architecture.
Inconsistent and Incomplete Data
When multiple systems collect similar information in different ways, you get inconsistent data. Different code sets, optional fields, and local documentation habits all affect downstream quality.
Common issues include:
• Missing or conflicting problem lists and medications
• Inconsistent use of diagnosis and procedure codes
• Unstructured text where structured fields are needed
• Duplicate patient records across facilities
These problems create healthcare data integration obstacles for analytics, care management, and reporting. Teams spend time performing manual data cleanup or reconciliations. Trust in the data erodes.
Latency and Timeliness of Data
Some workflows need near real time data. Others can use daily or weekly batches. When integration patterns do not match the use case, your teams experience delays or confusion.
For example:
• Care management teams need fresh ADT events and discharge data
• Operational leaders need timely census and throughput views
• Risk and quality teams need updated attribution and measure performance
If data arrives late or in inconsistent cycles, users question its value. This feeds the perception that data integration challenges in healthcare are unsolvable, even when the root issue is simply the wrong integration pattern for the job.
Security, Privacy, and Access Control
Large health systems must balance access to data with strict privacy and security obligations. As you increase connectivity, you increase the surface area for potential risk if not managed carefully.
Security related health system data integration issues include:
• Inconsistent access control models across systems
• Limited visibility into who accessed what data where
• Complex consent management for multi entity sharing
• Vendor and third party risk associated with data sharing
Security teams need assurance that integration patterns are standardized, monitored, and aligned with policy. Without that assurance, healthcare data governance challenges escalate and delay critical initiatives.
Strategies to Overcome Data Integration Challenges
You cannot remove all complexity in a large health system. You can reduce friction and risk with a structured, staged approach. Address technical, organizational, and data quality factors together. Treat integration as an enterprise capability, not a series of one off projects.
Standardize Around a Central Integration Platform
A modern integration platform creates a common foundation for interfaces, APIs, and data flows. Instead of point to point connections, you route traffic through a central hub with transformation, routing, and monitoring.
This approach helps you:
• Manage HL7, FHIR, and other formats in one place
• Reuse mappings and transformations across projects
• Monitor message flow and errors in a single console
• Scale integrations without linear increases in effort
As a result, core data integration challenges in healthcare become more manageable. You establish patterns that reduce variability and improve reliability.
Strengthen Data Governance and Ownership
Technology alone does not solve healthcare data governance challenges. You need clear roles and decision rights. Define data domains and owners. Create a data council with representation from clinical, operational, financial, and IT leaders.
Effective governance should:
• Define standard data elements and business definitions
• Prioritize integration work based on enterprise value
• Align security and privacy policies with use cases
• Set expectations for data quality and stewardship
This creates a framework to resolve health system data integration issues before they stall projects. It also supports consistent decision making as new use cases appear.
Invest in Data Quality and Identity Management
To reduce healthcare data integration obstacles caused by poor quality, invest in data quality and identity tools. Focus on patient, provider, and location identity first. Then expand to code sets, reference data, and clinical concepts.
A strong data quality strategy should:
• Standardize code sets and reference tables across systems
• Apply validation rules near the point of data entry
• Support ongoing monitoring of data quality metrics
• Provide workflows for correction and stewardship
These practices increase trust in analytics and operational data. They also reduce downstream rework on every new integration.
Align Integration Work with Strategic Outcomes
Data integration challenges in healthcare feel less overwhelming when you tie work to clear outcomes. Instead of tackling every interface problem at once, prioritize by impact.
Focus first on use cases that:
• Support enterprise quality and risk programs
• Improve care coordination for high need populations
• Support key financial and operational decisions
• Enable strategic digital health or consumer efforts
This lens helps leaders support necessary changes in workflow, governance, and technology. It also gives integration teams clear success measures.
Partner with Specialized Integration Experts
Many large health systems choose to partner with organizations that focus on healthcare integration full time. These partners bring repeatable patterns, proven tools, and specialized skills in HL7, FHIR, and complex vendor ecosystems.
The right partner helps you:
• Assess and rationalize your current integration landscape
• Design and implement a modern integration platform
• Standardize patterns across new and legacy systems
• Reduce risk during EMR transitions and mergers
This model reduces the burden on your internal teams and accelerates value from your data strategy.
Conclusion
Large healthcare system data integration is hard for predictable reasons. Fragmented systems, inconsistent standards, limited governance, and data quality gaps all compound into persistent integration delays and risk. You feel the impact in every strategic initiative that depends on connected data.
When you treat integration as a core enterprise capability, you start to break that cycle. A central integration platform, strong governance, structured data quality efforts, and outcome focused prioritization help you move beyond reactive projects. You reduce data integration challenges in healthcare to a manageable set of design choices, not constant firefighting.
Vorro helps large health systems build and run robust integration foundations that support clinical, operational, and financial outcomes. From HL7 and FHIR interfaces to complex multi vendor and multi entity environments, Vorro focuses on practical, reliable interoperability. If you want to reduce your healthcare data interoperability challenges and accelerate enterprise initiatives, connect with Vorro to align your integration strategy with your system’s goals.
FAQs
What are the biggest data integration challenges in healthcare for large systems?
Large systems struggle most with fragmented source systems, inconsistent standards, weak governance, and data quality issues. These factors combine into slow project delivery, unreliable analytics, and integration patterns that are hard to scale.
How do mergers and acquisitions affect health system data integration issues?
Mergers and acquisitions add new EMRs, billing, and ancillary systems into your environment. You inherit custom configurations, local standards, and unique workflows. Without an enterprise integration strategy, each new acquisition multiplies healthcare data integration obstacles and increases support complexity.
Why are healthcare data interoperability challenges so persistent?
Interoperability in healthcare involves more than technical standards. It requires aligned governance, consistent data definitions, and clear incentives for vendors and partners. Legacy systems, custom workflows, and strict privacy rules all make standardization difficult without focused effort.
How can strong governance reduce healthcare data governance challenges?
Strong governance defines who owns which data, sets common definitions, and aligns integration work with enterprise priorities. It gives security and compliance teams a clear framework, which reduces friction and speeds approvals for new data flows and use cases.
When should a health system consider a dedicated integration partner?
You should consider a partner when your internal teams face growing backlogs of integration work, frequent production issues, or large transformations such as EMR changes or expansion into new markets. A specialized partner brings repeatable patterns and tools that reduce risk and time to value.
