By manoj.kumar · January 20, 2026
Population health analytics sits at the center of every serious effort to improve outcomes and lower costs. You feel the pressure from value based contracts, clinical quality measures, and patients who expect coordinated care. Yet your data lives in silos, updates late, and rarely aligns across systems.
You do not have a data problem. You have an integration problem. Until you connect clinical, financial, operational, and social data into a single, trusted view, population health analytics will lag behind decisions.
This is where integrated healthcare data changes the equation. With a reliable integration layer, you turn scattered data into actionable healthcare data insights that support population health management, clinical analytics, and operational planning.
Population Health Overview
Population health analytics focuses on groups, not single encounters. You look across panels, cohorts, and communities to understand risk, gaps in care, and outcomes. When you do this well, you move from reactive care to proactive management.
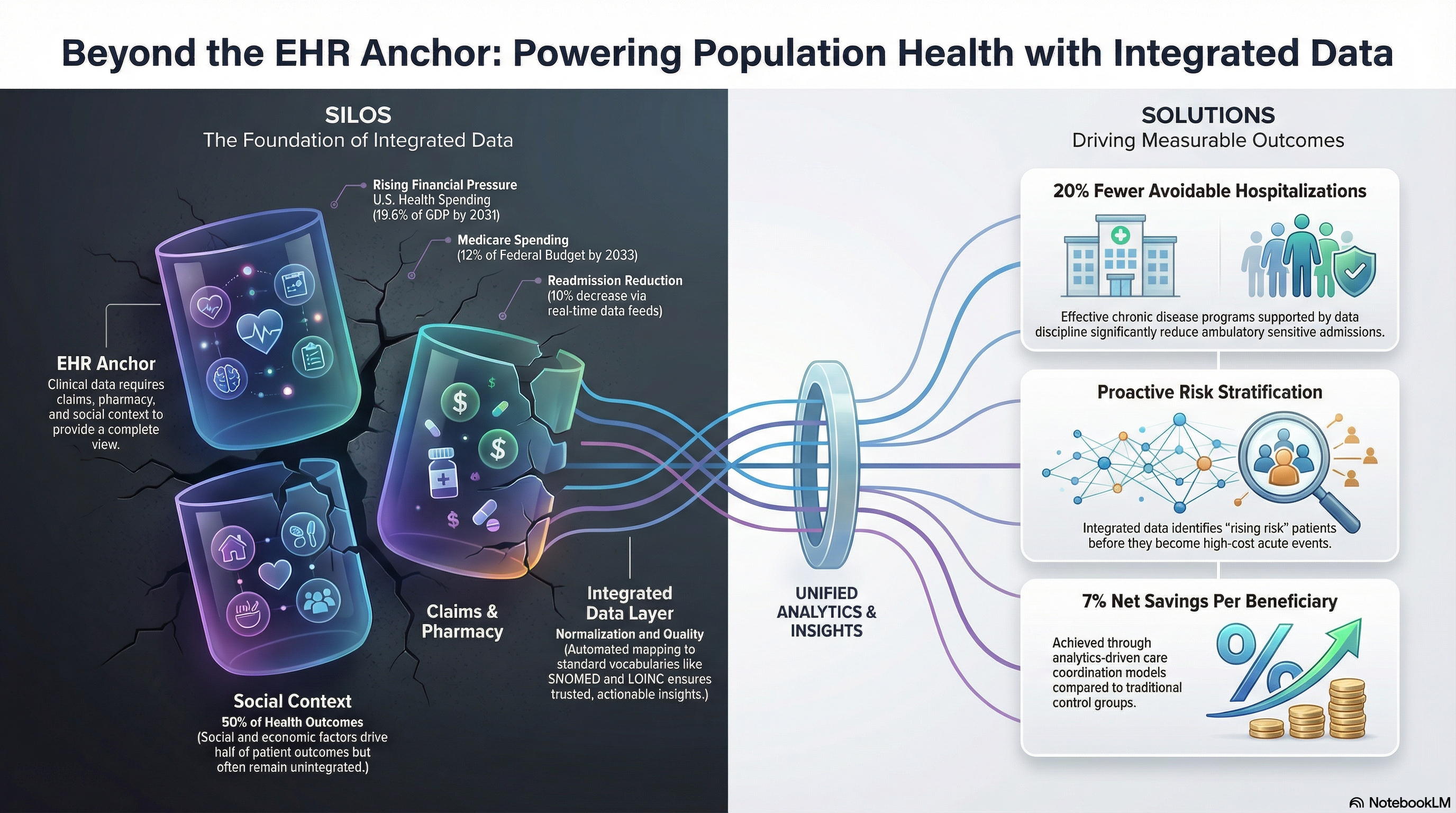
Health systems that lean into population health feel the financial impact. One analysis from the Agency for Healthcare Research and Quality linked effective chronic disease programs to a reduction of up to 20 percent in avoidable hospitalizations for ambulatory care sensitive conditions. That level of reduction requires both clinical insight and data discipline.
You also respond to a clear cost signal. The Centers for Medicare & Medicaid Services projects U.S. health spending to reach nearly 19.6 percent of GDP by 2031. Without targeted population health management, those dollars flow into acute events instead of early interventions.
Strong population health analytics gives you three things:
• Clarity on who is at risk and why.
• Insight into which interventions influence outcomes.
• Evidence to design and negotiate value based programs.
Each of those depends on integrated healthcare data, not isolated reports from single systems.
Data Sources
Population health analytics only performs as well as your data inputs. If any key source is missing or stale, insights lose precision. You need breadth across clinical, financial, behavioral, and social data. You also need depth, with enough history and granularity to see patterns over time.
Core clinical sources
Your EHR remains the anchor for clinical analytics. It provides diagnoses, medications, lab results, problem lists, allergies, care plans, and clinician notes. Yet EHR data alone cannot support robust population health management. It needs context from several other feeds:
• Claims data for complete cost and utilization history.
• Pharmacy data for adherence and polypharmacy risk.
• Lab and imaging systems for trend level clinical markers.
• Care management platforms for program engagement details.
Claims, cost, and utilization
Claims data fills in every encounter, not only those inside your walls. It includes out of network visits, urgent care, behavioral health, and ancillary services. Population health analytics depends on this view to understand total cost of care and to stratify risk accurately.
Health plans use similar information to manage risk scoring. The CMS Hierarchical Condition Category model shapes payment and incentives. Risk adjusted models influence billions of dollars in Medicare Advantage payments every year, with total Medicare spending projected to reach 12 percent of the federal budget by 2033. Integrated healthcare data helps you align clinical documentation with those models and avoid gaps.
Social and behavioral data
Population health management breaks down if you ignore social drivers of health. Transportation, housing, food access, and social support strongly influence outcomes. The World Health Organization estimates that social and economic factors account for up to 50 percent of health outcomes.
To incorporate this into healthcare data insights, you draw from:
• Screening tools in the EHR.
• Community based organization data feeds.
• Public datasets for neighborhood level indicators.
• Patient reported data from engagement tools.
Operational and quality systems
Your operational systems also matter for population health analytics:
• Scheduling and access data shows appointment lead times and no show risk.
• Quality reporting systems track measure performance and gaps in care.
• Patient experience platforms surface access and communication issues.
Without integration, each source adds friction. With integration, they form a unified picture that supports precise clinical analytics and strategy.
Integration Role
Reliable integration is the bridge between raw data and population health analytics. You need more than point to point interfaces. You need a governed integration fabric that connects systems, standardizes data, and keeps feeds current.
From silos to a unified data layer
Integrated healthcare data starts with connectivity. Modern integration platforms use standards such as HL7, FHIR, X12, and REST APIs to move data between EHRs, claims systems, CRMs, HIEs, and analytics tools. A single integration layer reduces the custom interface sprawl that slows most IT teams.
Interoperability also carries a clear regulatory push. The Office of the National Coordinator’s information blocking rules support patient access and system interoperability. At the same time, a 2023 ONC analysis found that about 70 percent of office based physicians electronically share patient health information outside their organization, which highlights both progress and remaining fragmentation. Integrated healthcare data helps you turn that external exchange into reliable internal analytics.
Normalization, matching, and quality
Integration is not only movement. It is also transformation and stewardship. To trust population health analytics, you need:
• Terminology mapping to standard vocabularies such as SNOMED, LOINC, and RxNorm.
• Master patient index and entity matching across systems.
• Data validation rules and quality scorecards.
• Metadata to track provenance, refresh timing, and use constraints.
When your data platform applies these steps continuously, you reduce manual cleanup, shorten analytics cycles, and free your teams to focus on clinical analytics and program design.
Near real time feeds for timely action
For population health management, timing matters. Daily or even hourly feeds let you respond to ED visits, inpatient admissions, and care gaps while they are still actionable.
Health systems that implement event based alerts tied to population health analytics often see measurable impact. One multi hospital study reported a 10 percent reduction in 30 day readmissions after implementing real time discharge and follow up workflows supported by integrated data. When your data arrives on time, your care teams can act on it.
Insights & Outcomes
Integrated healthcare data transforms population health analytics from retrospective reporting into a driver of day to day operations. The value appears in three main areas: risk, gaps, and performance.
More accurate risk stratification
When you join clinical, claims, and social data, you classify risk with higher precision. You see:
• Patients with rising risk, not only those already high risk.
• Members with frequent ED visits across multiple health systems.
• Individuals whose social needs undercut clinical progress.
Accurate risk stratification lets you align resources with need. Care managers can focus on segments where outreach influences both outcomes and cost. Actuarial and finance leaders can align contracts, stop loss coverage, and reserves with the real risk profile of your populations.
Closing care gaps and supporting adherence
Population health analytics also improves care gap closure. When your integrated data platform feeds care management and point of care tools, clinicians see open gaps inside their workflow, not in a separate report.
Evidence continues to support this link. Studies have found that integrated electronic reminders and outreach workflows raise vaccination and screening rates by 5 to 20 percent across different measures and populations. Integrated healthcare data underpins these reminders with accurate eligibility and history.
Targeted interventions and program design
Strong healthcare data insights help you test and refine interventions. You can:
• Compare telehealth, in person, and hybrid visit models for specific cohorts.
• Evaluate remote monitoring programs for high risk chronic disease groups.
• Measure the impact of community health worker visits on ED utilization.
This moves population health management into a continuous improvement cycle. Each program launch feeds new data into your analytics environment. Your integrated platform then surfaces outcome and cost signals, and you adjust accordingly.
Operational and financial performance
Population health analytics also influences operations and finance. When integration connects scheduling, throughput, and clinical outcomes, you can:
• Align clinic templates with demand from high risk panels.
• Size care management teams based on workload rather than averages.
• Track the margin impact of specific quality and utilization changes.
A study in Health Affairs reported that care models that integrated analytics driven care coordination achieved net savings of about 7 percent per beneficiary relative to control groups in certain value based programs. While results vary, the pattern is consistent. Better integrated data supports more precise operational decisions.
Conclusion
Population health analytics depends on a simple idea. You need the right data, in the right structure, at the right time, for the right teams. The difficulty comes from the number of systems, standards, and stakeholders involved.
When you invest in integrated healthcare data, you give clinicians, care managers, and executives a shared source of truth. That shared view supports targeted outreach, better clinical analytics, and more sustainable value based performance.
Vorro helps you reach that point faster. Vorro’s integration platform connects your clinical, financial, and community data into a single, secure, and governed layer that supports population health management, healthcare data insights, and analytics at scale. If you are ready to turn fragmented feeds into trusted population health analytics, schedule a conversation with Vorro.
FAQs
What is population health analytics?
Population health analytics is the practice of using data from multiple sources to understand and improve the health of defined groups of patients. You aggregate and analyze information from EHRs, claims, social drivers of health, and operational systems. You then use those insights to design care models, outreach strategies, and value based programs.
How does integrated healthcare data support population health management?
Integrated healthcare data connects clinical, claims, social, and operational systems into a unified data layer. This lets you stratify risk, track care gaps, and measure outcomes across settings and time. Population health management teams use this view to prioritize outreach, coordinate care, and monitor program performance without manual data extraction.
Which data sources are most important for effective population health analytics?
You gain the most impact when you combine four categories of data. These are EHR clinical data, payer and claims information, social drivers of health and community data, and operational and quality reporting systems. Together, these sources provide enough context to understand risk, behavior, and outcomes across the full care continuum.
What role does clinical analytics play in population health?
Clinical analytics focuses on patterns in diagnoses, treatments, labs, medications, and outcomes. Within population health, it helps you identify which interventions work for specific cohorts, where variation exists, and how care pathways influence cost and quality. Integrated data ensures that clinical analytics reflects the full patient journey, not only single episodes within one system.
How does Vorro help with healthcare data insights?
Vorro provides an integration platform that connects EHRs, claims systems, HIEs, community data, and analytics tools. It standardizes and delivers this information in a consistent structure that analytics and population health teams can trust. With Vorro in place, you reduce manual data work, shorten time to insight, and support population health management with a stable data foundation.
